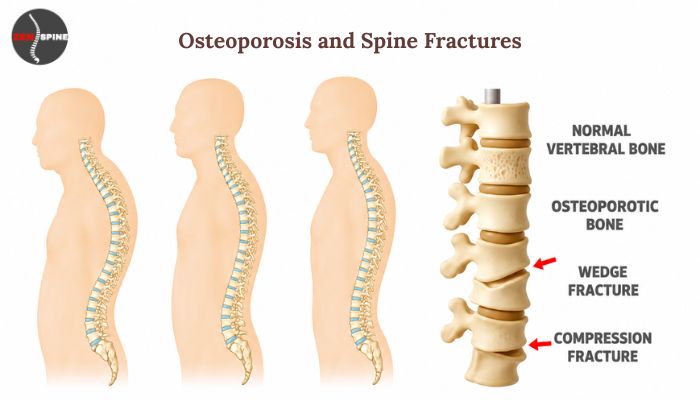
Spine fractures linked to osteoporosis often develop silently. Many patients do not recognize the problem until back pain becomes persistent or posture begins to change. This delayed recognition can affect long term spine health. With early awareness and timely care, these fractures can often be prevented or managed effectively.
Osteoporosis and the Spine: What Really Happens Inside the Bone
Osteoporosis is not just about weak bones. It is a gradual reduction in bone density and internal strength, making the skeleton less resilient to everyday stress. The vertebrae in the spine are especially sensitive to this change because they support body weight continuously.
In simple terms, healthy bone maintains a balance between breakdown and rebuilding. In osteoporosis, this balance shifts. Bone loss outpaces formation, leading to porous and fragile vertebrae. This condition is commonly seen in postmenopausal osteoporosis but can affect men and younger individuals with risk factors.
Clinical data from the World Health Organisation and International Osteoporosis Foundation show that low bone density is a leading contributor to fragility fractures worldwide. Many patients first discover osteoporosis only after a fracture occurs.
Compression Fracture Spine: A Common Yet Overlooked Injury
A compression fracture spine condition occurs when a weakened vertebra collapses. Unlike fractures caused by major trauma, these can occur during routine activities such as bending forward or lifting light objects.
The underlying spinal compression fracture causes are often linked to osteoporosis, where the bone is unable to withstand normal mechanical load.
Early Symptoms Patients Should Not Ignore
- Persistent mid or lower back pain that worsens with movement
- Gradual decrease in height over months or years
- Development of a rounded or stooped posture
- Reduced flexibility or difficulty standing upright
These osteoporosis symptoms and spine related changes may seem subtle but often indicate structural changes in the vertebrae.
Risk Factors of Osteoporosis Spine Fractures
- Age above 50, with increasing risk over time
- Hormonal changes associated with postmenopausal osteoporosis
- Low intake of calcium and vitamin D
- Limited physical activity and prolonged sitting habits
- Smoking and regular alcohol consumption
- Family history of osteoporosis or prior fractures
- Long term use of medications such as corticosteroids
Recognising these risk factors allows early intervention and reduces the need for complex vertebral fracture treatment later.
Why Vertebrae Become Vulnerable
Bone is a living tissue that constantly remodels itself. In osteoporosis, the internal structure becomes thinner and less connected. This weakens the vertebral body, making it prone to microdamage.
Over time, repeated stress leads to collapse. This is why back pain due to osteoporosis can appear without any clear injury. If left unaddressed, multiple fractures can lead to spinal deformity and reduced lung capacity due to posture changes.
Diagnosis and Bone Health Assessment in Mumbai
Evaluating osteoporosis spine fractures requires a combination of clinical examination and imaging studies. The most important investigation for assessing bone strength is the DEXA scan, also known as Dual Energy X ray Absorptiometry.
A DEXA scan measures bone mineral density and helps identify low bone density before fractures occur. It is considered the gold standard for diagnosing osteoporosis and estimating future fracture risk. Patients with persistent back pain, height loss, or risk factors for fragility fractures are often advised to undergo a bone density test in Mumbai for early detection.
Along with DEXA evaluation, spinal X rays may identify compression fractures, while MRI scans help determine the age of the fracture and assess surrounding soft tissue involvement.
At Zenspine, diagnosis focuses not only on detecting the fracture but also on understanding the underlying bone health condition to guide long term treatment planning.
Prevention Steps for Stronger Bones
- Ensure adequate calcium and vitamin D through diet, sunlight exposure, or supplements
- Follow a consistent routine of weight bearing and resistance exercises
- Schedule periodic bone density evaluations, especially after midlife
- Reduce fall risks at home by improving lighting and flooring safety
- Avoid tobacco use and limit alcohol intake
These spine fracture prevention strategies are strongly supported by global clinical guidelines and form the foundation of bone health management.
Treatment Approaches for Osteoporosis Spine Fractures
Treatment depends on the severity of the fracture, level of pain, and overall bone health.
Conservative Management
Initial care focuses on pain control, activity modification, and guided physiotherapy. Spinal bracing may be used temporarily to support healing.
Medical Treatment for Bone Strength
Osteoporosis treatment in Mumbai includes medications that improve bone density and reduce future fracture risk. These may include bisphosphonates and other therapies, along with calcium and vitamin D supplementation.
Minimally Invasive Procedures
When pain persists or vertebral collapse is significant, procedures such as vertebroplasty or kyphoplasty procedure are considered. These techniques stabilize the vertebra internally and can improve function.
How Treatment Decisions Are Made
Treatment is not the same for every patient. Factors include:
- Number and severity of fractures
- Bone density levels
- Functional limitations
- Overall health status
In clinical practice, Dr. Rakesh Dhake, a spine specialist in Mumbai, emphasises individualised care plans that address both immediate pain and long term bone stability.
What Happens If Osteoporosis Spine Fractures Are Ignored
Untreated fractures can lead to progressive spinal curvature, chronic pain, and reduced mobility. In advanced cases, multiple vertebral collapses may affect breathing capacity and daily function.
Early intervention helps prevent this cycle and improves quality of life.
A Personalized Approach at Zenspine
At Zenspine, patient care focuses on identifying the root cause of spinal weakness rather than only managing symptoms. Evaluation includes detailed clinical assessment, imaging, and bone health analysis.
Dr. Rakesh Dhake, Spine Specialist in Mumbai, integrates evidence based treatment with patient specific planning. The aim is to reduce fracture risk, restore function, and support long term spine health.
When Should You Seek Evaluation
Back pain that persists beyond a few weeks, unexplained height loss, or visible posture changes should not be overlooked. These signs may indicate early osteoporosis spine fractures.
Timely evaluation allows appropriate treatment before multiple vertebrae are affected, reducing long term complications.
Frequently Asked Questions
Q1. Can osteoporosis spine fractures heal on their own?
Answer: Some compression fractures heal with conservative care, but underlying osteoporosis still requires treatment to prevent recurrence.
Q2. Is every compression fracture painful?
Answer: No. Some fractures remain mild or painless initially and are detected during imaging for other concerns.
Q3. How effective is osteoporosis treatment?
Answer: With consistent treatment and monitoring, bone density can improve and fracture risk can be significantly reduced.
Q4. What is the role of vertebroplasty in osteoporosis spine fractures
Answer: Vertebroplasty is a minimally invasive procedure used in selected patients with painful vertebral compression fractures that do not improve with conservative treatment. During the procedure, medical bone cement is injected into the fractured vertebra to stabilize it and reduce pain. It is usually considered when persistent pain affects mobility and daily activities.
Q5. Can younger individuals develop osteoporosis?
Answer: Yes, especially in cases of nutritional deficiency, hormonal imbalance, or long term inactivity