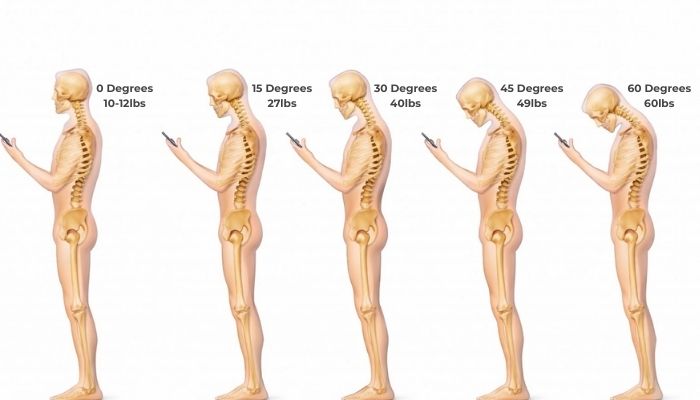
Persistent back or neck pain can slowly affect daily life. Simple tasks like sitting at a desk, walking, or sleeping comfortably may become difficult when the spine is unstable or damaged. Many patients try medicines, physiotherapy, posture correction, and lifestyle changes first. When these treatments do not bring relief, doctors may consider spinal fusion surgery.
A common question patients ask during consultation is about Minimally Invasive Spinal Fusion vs Traditional Fusion. Both surgeries aim to stabilise the spine and reduce pain, yet the surgical approach and recovery experience can differ.
Patients searching for the best spine surgeon for minimally invasive spine surgery often look for specialists who focus on modern surgical techniques that reduce tissue damage and support quicker recovery. Surgeons such as Dr. Rakesh Dhake, known by many patients as the best spine surgeon in mumbai, treat spine conditions using both minimally invasive and traditional surgical methods depending on the patient’s condition.
Understanding how these procedures differ can help patients make informed decisions about their spine care.
Understanding spinal fusion surgery
Spinal fusion surgery joins two or more vertebrae in the spine so that they heal as a single stable bone. Surgeons place a bone graft between the affected vertebrae and secure the area using implants such as screws or rods.
When the bones fuse together over time, painful movement between the vertebrae reduces. This stabilisation often helps relieve nerve pressure and chronic back pain.
Doctors may suggest spinal fusion surgery for several spine conditions, including degenerative disc disease, spinal instability, slipped disc that causes nerve compression, or spondylolisthesis where one vertebra shifts forward over another. The procedure may also be used in some cases of spinal deformity.
The goal of spinal fusion is not simply to remove pain but to restore stability so that the spine can function without abnormal movement.
Why spinal fusion becomes necessary for some patients
The spine contains discs that act as shock absorbers between vertebrae. With age or injury, these discs may wear out, bulge, or slip from their normal position. When this happens, the vertebrae may move abnormally or press on nearby nerves.
Patients may then experience ongoing symptoms such as lower back pain, pain radiating to the legs or arms, numbness, tingling sensations, or muscle weakness. In some cases walking or standing becomes difficult because nerve compression causes sharp or burning pain.
Doctors usually start with non surgical treatments such as physiotherapy, medicines, posture correction, and lifestyle adjustments. If these methods do not control symptoms or if spinal instability worsens, spinal fusion surgery may be considered.
At this stage many patients want to understand the difference between open and minimally invasive spinal fusion.
What is minimally invasive spinal fusion?
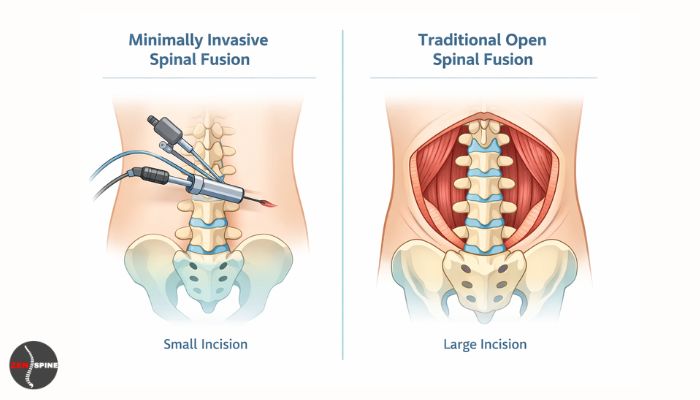
Minimally invasive spinal fusion uses smaller skin openings and specialised surgical instruments to reach the spine. Instead of making a large incision, the surgeon creates small entry points through which surgical tools and imaging equipment guide the procedure.
The muscles around the spine are gently moved aside rather than cut. This approach reduces tissue damage around the surgical area. Surgeons then place implants such as screws and rods to stabilise the spine and allow bone fusion to occur over time.
Because the surrounding tissues remain largely preserved, many patients experience less post operative discomfort and a smoother recovery compared with traditional surgery. These minimally invasive spine surgery advantages have made the technique increasingly common in modern spine care.
What is traditional open spinal fusion?
Traditional spinal fusion surgery uses a larger incision along the back to expose the affected section of the spine. The surgeon moves the muscles away from the spine to obtain a clear view of the surgical area.
This direct exposure allows the surgeon to perform complex procedures when several vertebrae are involved or when spinal deformity requires correction. Traditional surgery has been used for many years and continues to be effective for complicated spinal problems.
However, because the procedure involves a larger incision and greater muscle disturbance, recovery can take longer in some patients.
Difference between open and minimally invasive spinal fusion
Patients often want a simple explanation of open spinal fusion vs minimally invasive surgery. The two procedures aim to stabilise the spine, but the surgical technique and recovery experience can differ.
| Factor | Minimally Invasive Spinal Fusion | Traditional Open Spinal Fusion |
| Incision | Small skin openings | Larger incision along the back |
| Muscle impact | Muscles gently separated | Muscles moved away from the spine |
| Blood loss | Usually lower | Usually higher |
| Hospital stay | Often shorter | Often longer |
| Recovery | Faster early recovery for many patients | Recovery may take longer |
| Surgical exposure | Guided with imaging technology | Direct visual access to spine |
Understanding this difference between open and minimally invasive spinal fusion helps patients discuss treatment options with their surgeon more confidently.
Minimally invasive spinal fusion benefits
Many patients ask why surgeons increasingly use minimally invasive techniques. One reason involves the reduced disturbance to surrounding tissues.
Because the surgical openings are smaller, the muscles around the spine remain largely intact. This often leads to lower blood loss during surgery and less discomfort after the procedure. Patients may also regain mobility sooner because the muscles do not require extensive healing.
Another important benefit involves hospital stay. Many patients undergoing minimally invasive surgery are able to leave the hospital earlier than those who have traditional open surgery.
These advantages contribute to the growing popularity of minimally invasive techniques for appropriate spinal conditions.
Traditional spinal fusion surgery risks
Although traditional spinal fusion remains an effective treatment, it can involve certain risks due to the larger surgical exposure.
The muscles surrounding the spine may take longer to recover because they are moved away from the surgical area during the procedure. This can result in increased post operative pain during the early stages of recovery.
Traditional surgery may also involve greater blood loss and a longer hospital stay compared with minimally invasive procedures. These traditional spinal fusion surgery risks are one reason why surgeons consider minimally invasive techniques whenever the patient’s condition allows.
However, in cases involving complex spinal deformities or multi level instability, traditional surgery may still provide the safest approach.
Recovery timeline after spinal fusion
Patients preparing for surgery often want to know what recovery may look like. While recovery differs for each individual, a general spinal fusion surgery recovery timeline can help patients understand the process.
During the first one or two days after surgery, patients usually begin gentle movement and short walks with medical guidance. Early movement helps reduce stiffness and improves circulation.
Within the first few weeks, many patients gradually increase their daily activities. Light household tasks and short walks often become easier as healing progresses.
Over the next two to three months, the spine continues to stabilise while the bone fusion develops. Doctors may suggest physiotherapy to improve strength and posture.
Full bone fusion usually develops gradually over several months. Following the surgeon’s instructions during recovery is essential for the best results.
Patients who undergo minimally invasive procedures often experience a smoother early recovery compared with traditional surgery.
Possible spinal fusion surgery complications
Every surgical procedure carries some degree of risk. Although complications are not common, patients should understand potential concerns before surgery.
Possible spinal fusion surgery complications include infection, bleeding, nerve irritation, or delayed bone fusion. In rare situations the implants used to stabilise the spine may require adjustment.
Choosing an experienced spine surgeon, maintaining good health before surgery, and following rehabilitation instructions after surgery all help reduce these risks.
Which procedure may be better for patients?
The answer to Minimally Invasive Spinal Fusion vs Traditional Fusion depends on the specific spinal condition.
Minimally invasive spinal fusion often offers advantages such as smaller incisions, reduced muscle disturbance, and faster early recovery. For many patients with limited spinal instability or degenerative disc disease, this technique provides effective results.
Traditional open surgery may still be necessary for complex spinal problems, severe deformities, or conditions involving multiple spinal levels.
A spine specialist evaluates imaging scans, symptoms, and overall health before deciding which surgical approach is most suitable.
Patients looking for the best spine surgeon for minimally invasive spine surgery often prefer surgeons with experience in modern spine procedures. Dr. Rakesh Dhake treats various spine conditions using patient specific treatment planning, which may include minimally invasive techniques when appropriate.
Final thoughts
Living with long term back or neck pain can affect physical health and daily comfort. When non surgical treatments do not provide relief, spinal fusion surgery may help restore stability and reduce nerve pressure.
Understanding the difference between open and minimally invasive spinal fusion allows patients to discuss treatment options more clearly with their doctor. Minimally invasive techniques often provide faster recovery and reduced tissue damage, while traditional surgery remains important for complex spinal conditions.
Consulting an experienced spine specialist is the best step toward understanding the right treatment plan. Patients experiencing persistent spine pain can consider evaluation by specialists such as Dr. Rakesh Dhake to learn whether minimally invasive spine surgery may be suitable for their condition.
Early diagnosis and proper treatment planning often lead to better recovery and improved quality of life
Frequently asked questions
What is the difference between minimally invasive spinal fusion and traditional fusion?
Minimally invasive spinal fusion uses small incisions and specialised instruments, while traditional fusion involves a larger incision to directly access the spine.
How long does minimally invasive spinal fusion recovery take?
Many patients start walking within one or two days. Light activities may resume within several weeks depending on healing and medical advice.
Is minimally invasive spinal fusion safer than traditional surgery?
For suitable patients it may reduce tissue damage and shorten recovery time, but the best method depends on the spinal condition.
What conditions require spinal fusion surgery?
Doctors may suggest spinal fusion for degenerative disc disease, spinal instability, slipped disc with nerve compression, or spondylolisthesis.
.